
Member Engagement
Members can engage with our program as they wish. The multi-faceted program meets the members where they are, and employers can customize their engagement program to meet the needs of their population.
Members deserve coordinated and connected care across the network.
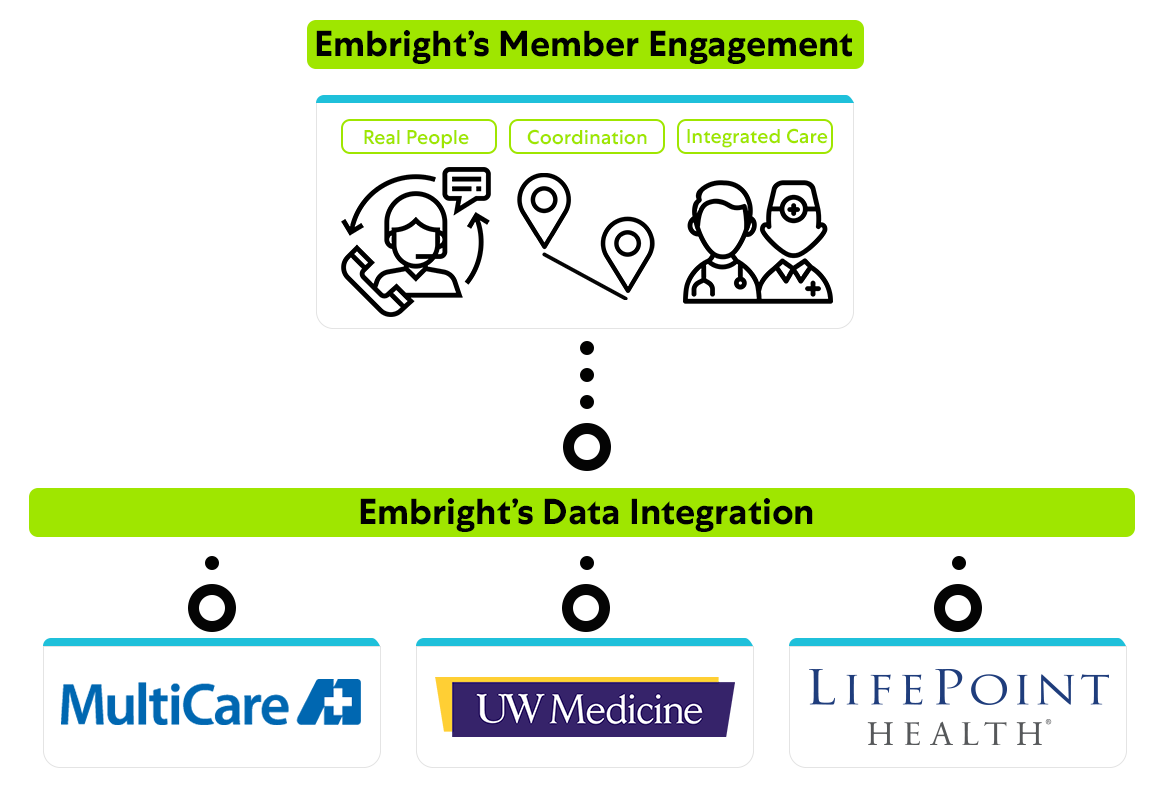
Enhanced navigation, access, and coordination
Members within our engagement program experience the refreshing feeling of a real person helping with their questions. On top of that, our member engagement program, powered by our integrated data, allows members to:
- Access in-network doctors, specialists, clinics, and hospitals across MultiCare Health System, UW Medicine, and LifePoint Health
- Experience coordinated care across these independent health systems resulting in fewer forms needed and valuable time saved
"You've been a great help and the [resource] links sent gave me better direction. Thanks for getting us going in the right direction, it's much appreciated."
Benefits to a fantastic member experience
Embright aims for each and every member's experience to be delightful, and that is saying a lot when it comes to traditional healthcare. Members expect more, and we aim to meet and exceed their expectations when it comes to navigating and accessing their health plan.

Delightful Interactions
Our member engagement program connects members with real people answering their questions. If self-service is the preferred method, our online, personalized portal and real-time chat can get a member the information they need quickly without the need to talk to anyone.

Coordinated Communication
We complement our health systems communication methods to ensure members get the appropriate communications about their care from the appropriate source.
.png)
Shared Savings
With a unified member profile available to those serving the member, members experience less waste such as the reduction or elimination of duplicative services resulting in money saved.
How the program works

Develop a meaningful communication strategy
We work with the employer to understand the communication preferences across the employee population and develop a strategy to engage with prospective members and enrolled members pre- and post-annual enrollment.

Coordinate with stakeholders and implement
Embright understands the different member communications planned across health systems and other parties. We work to ensure the member gets the appropriate communication from the appropriate source with the goal to eliminate duplicative communications.

Report out and continuously improve
Post-annual enrollment, Embright provides regular reports to the employer outlining call volumes, online interaction volumes, resolved questions, and wait times. Throughout the year, Embright works with the employer to ensure each and every member has a delightful experience.
"I just want to thank you so much for all your support and help in this matter. Your help really means the world to me and I really appreciate you."
Care coordination benefits all
Care coordinated across health systems and providers benefit the member, the employer, and the providers delivering care.